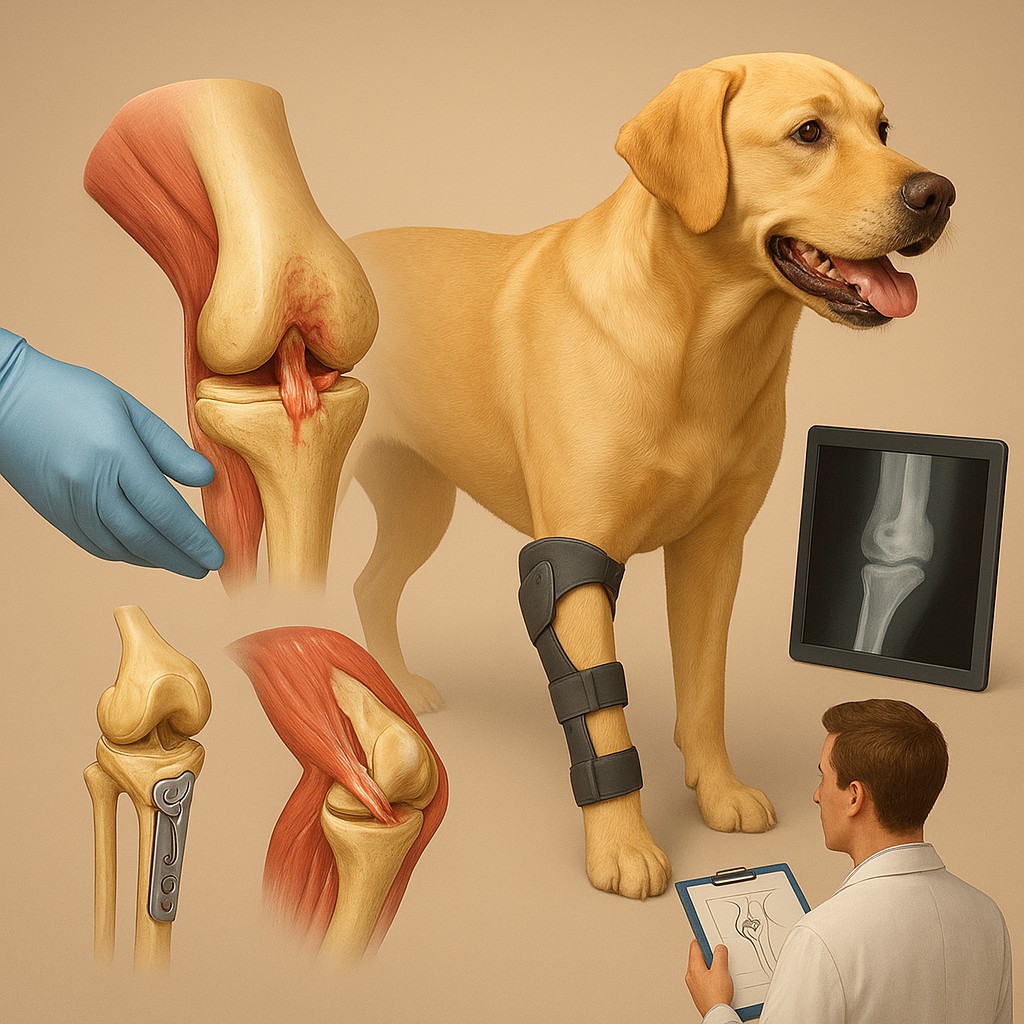
Your dog races after a tennis ball, twists midair like a nature show star, lands, and then suddenly holds up one hind leg as if it were made of glass. The limp might ease after a day or two, then come back with a vengeance after the next bout of “I am speed.” Many owners assume it is a simple sprain, or that rest will fix it. Sometimes rest helps, but one knee injury tends to hang around and quietly change your dog’s comfort and mobility: a torn ACL, which in dogs is usually called a torn CCL (cranial cruciate ligament).
This matters because the choices you make early on shape the next year. The question is not just “surgery or no surgery.” There are different surgical methods, braces that range from genuinely helpful to overhyped, and rehab plans that can make a great surgery even better or let a decent repair fall apart. Also, dogs are not small humans, and their knees do not follow human rules. The good news is that once you understand how a dog knee works, the treatment options stop feeling like vet magic and start to read like sensible mechanics.
We will cover what the ligament does, why it fails, how surgeries change the mechanics, how a brace compares, and what life is like after the procedure. By the end, you should be able to talk to your veterinarian or surgeon with confidence, ask better questions, and recognize what real recovery looks like.
The dog knee: a hinge with a built-in tendency to slide
A dog’s stifle joint, the knee, is where the femur (thigh bone) meets the tibia (shin bone). It is not a simple hinge. When a dog puts weight on the leg, forces try to push the tibia forward. The cranial cruciate ligament (CCL) is one of the main structures that stops that forward slide, which vets call cranial drawer or tibial thrust depending on how they test for it.
Here is the key detail that makes dog ACL injuries different from human ones: many dogs have a naturally sloped tibial plateau, the top of the tibia. When the knee is loaded, that slope tends to shove the tibia forward, even during normal walking. The CCL resists that. If the CCL is damaged, the tibia can slide forward each time the dog steps, which irritates the joint lining, strains other soft tissues, and speeds up arthritis.
CCL failure in dogs is often not a single dramatic snap like in human athletes. It can be a slow breakdown of the ligament fibers, starting with a partial tear and later becoming a full tear. That is why some dogs limp off and on for weeks, then suddenly get much worse. It also explains an annoying truth: fixing one knee does not eliminate risk in the other knee, because the same forces and genetics that damaged the first can affect the other later.
How to recognize a CCL tear and what diagnosis really involves
Dogs are great at acting fine until they are not. A classic sign is sudden hind-limb lameness, often with the dog touching the toe only or holding the leg up. Some dogs sit with the affected leg sticking out to the side. Others still bolt after a squirrel because pride matters, but they limp afterward and struggle with stairs or getting into the car.
Common signs owners notice include:
- Limping that improves with rest but returns with activity
- Stiffness after naps, like your dog is doing an impression of an old cowboy
- Trouble jumping or climbing stairs
- A “click” or “pop” sensation (sometimes from a meniscus injury)
- Muscle loss in the affected thigh over time
- A bit of swelling on the inside of the knee, called a medial buttress
Diagnosis usually combines the history, a physical exam, and sometimes imaging. Your vet may do a drawer test or a tibial thrust test to feel abnormal movement. Many dogs are tense or painful during the exam, so sedation can help the vet get a clearer answer. X-rays do not show the ligament itself, but they can show swelling, early arthritis, and rule out fractures or bone tumors. In some cases, advanced imaging or arthroscopy (a camera inside the joint) is used, especially when the diagnosis is unclear or to plan specific surgical steps.
A useful correction: if your dog can still walk on the leg, the ligament can still be torn. Partial tears are real, and they often progress. Another myth: “It is just old age.” Arthritis can cause stiffness, yes, but a CCL tear creates instability that usually speeds arthritis up, so treating the instability can change the arthritis course.
Braces, rest, rehab, and surgery: what each option is trying to accomplish
All treatment options aim for the same big goal: a stable, comfortable knee your dog can load without pain. They differ in how they try to get there.
A brace (orthosis) tries to mechanically limit abnormal movement and support the joint while scar tissue forms. Rest and rehab aim to lower inflammation, build muscle, and improve function without changing the bones. Surgery changes mechanics more directly, either by stabilizing the joint with an internal construct or by altering bone geometry so the knee no longer "needs" the ligament in the same way.
A clear comparison of brace vs surgery (and where conservative care fits)
Below is a practical comparison. Remember that results vary with dog size, activity level, tear severity, meniscus status, body condition, and how committed the household is to rehab. Yes, the household matters, because dogs do not drive themselves to physical therapy.
| Feature |
Surgery (TPLO/TTA/Extracapsular) |
Brace (custom orthosis) |
Conservative care (rest, meds, rehab) |
| Main goal |
Restore long-term functional stability |
Provide support, reduce instability, improve comfort |
Reduce pain, build muscle, manage without restoring true stability |
| Best suited for |
Most medium to large dogs, athletic dogs, complete tears, meniscus injury |
Some partial tears, dogs that cannot have surgery, short-term support |
Small dogs, very low-activity dogs, owners highly committed to rehab |
| Speed of functional improvement |
Often faster and more reliable once healing starts |
Variable, depends on fit, compliance, and tear severity |
Often slow, may plateau below desired function |
| Long-term arthritis control |
Usually better than instability-based options, arthritis still progresses |
Mixed; may help symptoms but instability can persist |
Mixed to poor if instability remains |
| Risks |
Anesthesia, infection, implant issues, meniscus injury, rehab setbacks |
Skin sores, poor fit, limited effectiveness, false confidence leading to overactivity |
Ongoing instability, chronic pain, muscle loss, higher chance of meniscus injury |
| Cost profile |
Higher upfront, may reduce long-term costs |
Moderate, may need adjustments or replacement |
Lower upfront, may increase long-term costs |
A key point: a brace is not always a replacement for surgery. For some dogs, it is a bridge to surgery, giving support while you schedule and prepare. For others, it is a permanent plan because surgery is not safe or possible. Braces need an excellent fit, consistent use, and careful skin checks. A brace that slips or rubs can trade knee pain for skin wounds, which is not an upgrade anyone wants.
The main surgical options and how they change the physics
Veterinary surgeons use several well-established techniques. They differ in how they address the central problem: the tibia wants to slide forward under load.
TPLO: changing the slope so the knee stops trying to slide
TPLO stands for Tibial Plateau Leveling Osteotomy. In plain terms, the surgeon cuts the top of the tibia, rotates it to reduce the slope, and fixes it in the new position with a plate and screws. By leveling the tibial plateau, the forward thrust during weight-bearing is reduced so the knee becomes stable during motion, even without a working CCL.
TPLO is widely used, especially for medium and large dogs, active dogs, and working breeds. It has a strong track record for returning dogs to high function. It does not replace the ligament, it redesigns the knee geometry so the ligament is less necessary for stability when the dog bears weight.
TTA: shifting forces by changing the patellar tendon angle
TTA stands for Tibial Tuberosity Advancement. Instead of rotating the tibial plateau, the surgeon moves the tibial tuberosity, where the patellar tendon attaches, forward and secures it with implants. This changes the angle of the patellar tendon to neutralize the forward thrust during weight-bearing.
TTA works well in appropriately selected patients, and different surgeons prefer different techniques based on training, dog anatomy, and case details. Like TPLO, TTA is a bone surgery with implants, which means it needs careful healing and controlled rehab.
Extracapsular repair and "tightrope" style techniques: stabilizing with a strong suture
Extracapsular techniques stabilize the knee by placing a strong material, often a heavy suture-like line, outside the joint to mimic the ligament. Think of it as an internal support line that limits abnormal motion while scar tissue forms and the dog adapts.
These procedures are often used for smaller or less active dogs, or when bone-cutting surgeries are not ideal. They can be very successful, but in large, athletic dogs, the forces may overwhelm the repair over time. That is not a failure of the surgery, it is just physics.
What about the meniscus?
The menisci are cartilage pads that act like shock absorbers and stabilizers in the knee. When the CCL tears, the abnormal motion can trap and tear the medial meniscus. This can cause persistent pain and sometimes a clicking sensation. During surgery, the surgeon usually inspects the meniscus and treats it if torn, often by removing the damaged portion. Treating a torn meniscus is one reason surgery can give a more complete solution than bracing alone, because a brace cannot remove a loose piece of cartilage inside the joint.
What actually happens on surgery day (in human-friendly terms)
Surgery day can be more emotionally intense for owners than for dogs. Dogs are experts at living in the moment. You, meanwhile, are imagining every possible outcome and staring at your phone like it owes you money.
A typical workflow goes like this: your dog is admitted, examined, and put under anesthesia with close monitoring of heart rate, breathing, blood pressure, oxygen, and temperature. Pain control is not an afterthought. Many clinics use multimodal pain management, meaning several types of medication and sometimes local nerve blocks to control pain from different angles. The surgical site is clipped and scrubbed carefully to reduce infection risk.
For TPLO or TTA, the surgeon does the bone cut, aligns the bone to the planned position, and secures it with implants. For extracapsular repair, the surgeon places the stabilizing line and checks knee stability. Many surgeons also look inside the joint, either through an arthrotomy (opening the joint) or arthroscopy (a camera), to examine the meniscus.
After surgery, your dog recovers from anesthesia in a warm, monitored area. You will usually go home the same day or after a short stay, depending on your dog’s health, pain control, and the clinic’s rules. You will also go home with instructions that make it clear you have adopted a small orthopedic patient, which, to be fair, you have.
The weeks after surgery: the part everyone underestimates
The most common recovery mistake is thinking the surgery “fixed it” so the dog can return to normal as soon as they seem happier. Dogs often feel better before they are truly healed, especially once pain meds and swelling go down. That is when the risk of setbacks goes way up.
The first two weeks: protect the repair, control inflammation, establish routines
Early recovery is about protection and consistency. Expect leash-only potty breaks, no running, no jumping, no stairs if you can avoid them, and definitely no “just one quick game of fetch.” Incision care matters, and so does preventing licking. Cones are not stylish, but neither are infected incisions.
You will likely use pain relief, anti-inflammatory medication when appropriate, and sometimes antibiotics depending on the surgeon’s protocol. Cold packs may be recommended early to reduce swelling, and gentle range-of-motion exercises may begin if your surgeon approves.
Weeks three to eight: gradual rebuilding, not a return to chaos
As healing progresses, your vet or rehab therapist will increase activity in a controlled way. This often includes longer leash walks, controlled sit-to-stand exercises, and strengthening work for the glutes and thigh muscles. Hydrotherapy, such as an underwater treadmill, can be especially helpful because it builds strength while reducing joint impact.
This phase is where physical therapy becomes more than a nice extra. It helps restore normal movement patterns, prevent compensation injuries, and rebuild muscle that protects the joint. A dog that learns to use the leg correctly is less likely to overload the other knee, the hips, or the lower back.
Months two to six: return to function, and then return to sport (if appropriate)
Bone healing after TPLO or TTA takes time. Many dogs look much better by 6 to 10 weeks, but that is not the finish line. Your surgeon will usually recommend recheck exams and follow-up X-rays to confirm healing before full activity is allowed. Off-leash running, jumping, and rough play are usually delayed until the surgeon is confident the bone and implants can handle it.
Even after “graduation,” keep a maintenance mindset: keep your dog lean, keep their muscles strong, and avoid bursts of weekend-warrior activity after long sedentary stretches. Dogs do not warm up like human athletes, and they do not read training plans.
Complications, reality checks, and myths worth retiring
No surgery is risk-free, but many risks are manageable when you know what to watch for and follow instructions like they are the map out of the jungle.
Possible complications include infection, implant problems, delayed bone healing, and meniscal tears that show up later. Some dogs have mild ongoing lameness or stiffness, especially if arthritis was already present. That said, many dogs return to an excellent quality of life, including hiking, running, and doing their jobs.
Let us toss a few myths into the recycling bin:
- Myth: "My dog is too old for surgery." Age alone is not the deciding factor. Overall health, mobility goals, pain, and anesthesia risk matter more than the number of birthdays.
- Myth: "A brace will heal the ligament." Ligaments inside joints have limited healing ability, especially with ongoing instability. A brace can support function and comfort, but it usually does not restore the original ligament.
- Myth: "If the limp is gone, we can stop rehab." The limp can fade before strength and coordination return. Stopping early raises reinjury risk and can create long-term compensation patterns.
- Myth: "Surgery prevents arthritis." Surgery can reduce abnormal motion and slow arthritis progression, but it does not reset the joint to a brand-new state.
A practical reality check: weight management is one of the strongest predictors of comfort after a CCL injury. Extra weight increases force through the knee and makes every step harder. If you want one bonus treatment that helps every plan, it is keeping your dog at a healthy body condition.
How to choose between surgery and a brace without losing your mind
Decision-making gets easier if you anchor it to a few concrete questions instead of drowning in internet opinions.
Questions that clarify the right path
- How big is my dog, and how active do we want them to be after recovery?
- Is this a partial tear or a complete tear, and is there suspected meniscus injury?
- What does my vet think about arthritis already in the joint?
- Are there health issues that make anesthesia or surgery unusually risky?
- Can our household realistically do strict confinement and structured rehab?
- Do we have access to a surgeon experienced in the procedure being recommended?
Generally, surgery is often recommended for medium to large dogs, very active dogs, complete tears, and cases where long-term stability is the priority. Bracing may be considered when surgery is not possible, when the tear is partial and the dog’s needs are modest, or as short-term support while planning surgery. Conservative care can work best for small, calm dogs, especially when owners are diligent about rehab and weight control, but it may not provide the stability many larger dogs need.
The comeback story: what “success” really looks like
A successful recovery is not just “walking without limping.” It is a dog that uses the leg naturally, rebuilds muscle, and returns to joyful movement without frequent flare-ups. It is also an owner who understands that healing is a process, not an event. The surgery is one day, but the outcome is built over weeks of careful choices, boring leash walks, and the occasional triumph when your dog finally hops into the car without hesitation.
If you are facing this decision now, take heart: CCL injuries are common, the treatments are well-studied, and veterinary orthopedics has come a long way. With the right plan, good pain control, and thoughtful rehab, many dogs return to the activities that make them feel like themselves. Your job is not to become an orthopedic surgeon overnight, it is to be the steady teammate who follows the plan when your dog is feeling spicy and thinks rules are optional. Stay patient, stay consistent, and you will be amazed at how strong a dog can become when healing gets time and structure.