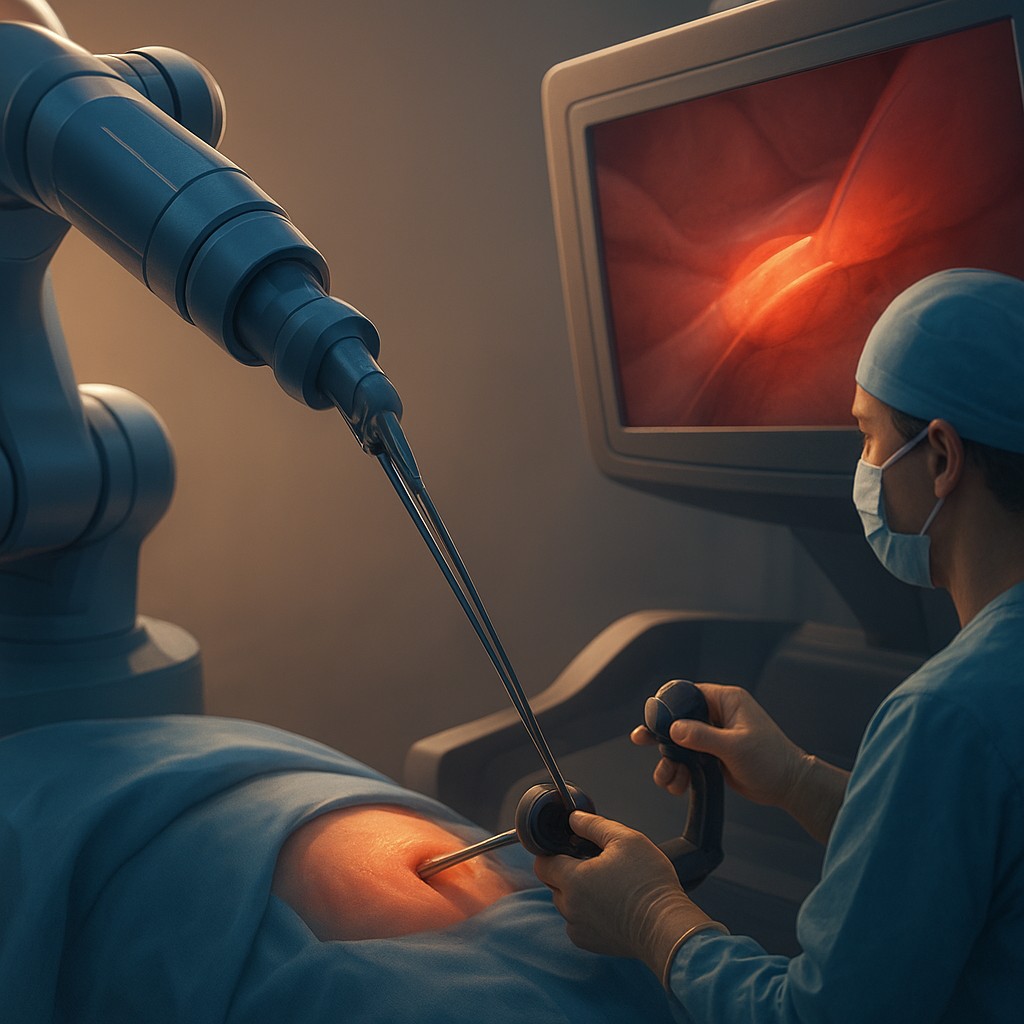
Imagine trying to tie your shoelaces while wearing thick winter mittens, or perhaps icing a cupcake with a pair of long BBQ tongs. You can see the string or the frosting clearly, but the vital connection between your fingertips and the material is gone. This is the central problem that has haunted robotic surgery for decades. While robots have given surgeons superhuman precision, 3D vision, and the ability to operate through tiny cuts, they stripped away one of the healer's most basic tools: the sense of touch.
Without tactile feedback, a surgeon at a remote console is essentially flying blind. They rely entirely on "visual haptics," a fancy way of saying they watch for tissue to move or thread to pull tight to guess how much pressure they are applying. If the tissue bulges too much, they are pushing too hard; if the thread snaps, they have gone too far. Depending on sight alone is mentally exhausting and leaves room for error. Delicate vessels can be crushed or internal bruising can occur simply because the doctor couldn't "feel" the resistance of the organ they were handling.
The Invisible Engine of Digital Touch
To bridge this gap, engineers have developed a field called haptic rendering. This is not just a single piece of hardware, but a complex system of "force-feedback" loops that turn mechanical resistance into human sensation. At the working end of the robot, inside the patient’s body, sensitive sensors are built into the surgical tools. These sensors are incredibly precise, measuring the tiny units of force, known as Newtons, exerted as a needle pierces a muscle or a gripper holds a vein. This data is converted into digital signals and sent back to the surgeon’s console instantly.
Once the data reaches the console, the "rendering" part begins. Inside the hand controllers the surgeon moves are small, high-precision motors called actuators. These motors create physical resistance against the surgeon’s fingers. If the robotic arm hits a stiff piece of scar tissue, the motors in the controller push back, making it harder for the surgeon to move their hand forward. If the tissue is soft, the motors offer little resistance. This creates a seamless illusion where the surgeon feels as though they are physically touching the patient, even if they are several feet or even miles away.
Turning Physics into Calculated Feeling
The magic of haptic rendering lies in how it sorts different types of physical contact. It is not just about "pushing back." To make the experience feel real, the software must tell the difference between various materials. Engineers use math models to define how certain "virtual" objects should feel. For example, when a surgeon hits a solid boundary like bone, the system uses a "penalty-based" model, where the resistance ramps up the moment the tool makes contact. This stops the surgeon from accidentally moving too far into a restricted area.
Beyond simple resistance, haptic rendering can also simulate texture and vibration. This is the difference between "tactile" and "kinesthetic" haptics. Kinesthetic feedback tells you about the position and weight of an object, while tactile feedback tells you about the surface. Modern systems can simulate the "grittiness" of a kidney stone or the pulsing of an artery. By combining these sensations, the robot provides a multi-sensory map of the surgery site. This allows the surgeon to tell the difference between healthy tissue and a firm tumor purely by touch - a process called palpation that many feared would be lost with robotic surgery.
| Feature of Haptic Feedback |
Mechanical Mechanism |
Clinical Benefit |
| Stiffness Rendering |
Motors push against the controller based on tissue density. |
Prevents piercing organs and helps find tumors. |
| Friction Simulation |
Tiny vibrations in the controller simulate surface texture. |
Keeps stitches from slipping and improves the grip on wet tissue. |
| Force Scaling |
Sensors amplify tiny forces so human hands can feel them. |
Allows for extreme delicacy when working on microscopic vessels. |
| Virtual Boundaries |
Software creates "No-Go" zones that physically stop the controller. |
Protects critical areas like the spinal cord or major arteries. |
The Challenge of Living in the Near-Present
While haptic rendering is a breakthrough, it still faces technical hurdles, the biggest being "latency" or delay. In a perfect world, the moment the robotic arm touches a lung, the surgeon would feel it. However, in reality, data must be processed, sent, and turned into motor movement. This creates a tiny delay, often measured in milliseconds. While a hundred-millisecond delay sounds fast, it can create a "stutter" in the feedback loop during surgery. If the doctor reacts to a sensation that happened a fraction of a second ago, they might over-correct, leading to a shaky movement called "instability."
Surgeons must develop a specific type of muscle memory to handle this. They learn to operate in the "near-present," slightly anticipating the feedback they are about to receive. Engineers are currently working on "predictive haptics," where AI models guess the resistance based on where the tool is moving. This effectively "fills in" the delay gap so the sensation feels instant. This balance between human intuition and machine processing makes modern robotic surgery a true partnership between man and code.
Redefining the Boundaries of Surgical Safety
Adding simulated touch does more than just make the surgeon feel comfortable; it fundamentally changes how safe an operation is. When a surgeon can feel the tension in a stitch, they can tighten it perfectly without damaging the tissue. This leads to faster healing and fewer complications after surgery. Furthermore, haptic systems can be programmed with "safety ceilings." If a tired surgeon applies a force that the software considers dangerous, the system can vibrate an alert or even "lock" the movement to prevent injury.
This technology also makes training much better. In the past, a student had to watch a mentor and guess how much pressure they were using. With haptic rendering, a teacher and a student can be linked on two consoles. The student can "feel" the exact amount of tension the master surgeon uses during a difficult move. This "haptic shadowing" speeds up learning by turning a visual lesson into a physical one. As we look to the future, adding touch to the digital workspace ensures that as our tools become more robotic, our connection to the patient remains deeply human.
The evolution of surgery has always been a journey of getting closer to the problem - first with large cuts, then with cameras, and now with sensors that go beyond the limits of our own skin. By bringing back the sense of touch through haptic rendering, we are not just adding a feature to a machine; we are restoring a surgeon’s most vital instinct. As these systems improve and delays shrink, the line between the cold steel of the robot and the warm hand of the doctor will continue to blur, making the "impossible" surgeries of yesterday a routine success tomorrow. Through the marriage of physics and digital empathy, we are ensuring the future of medicine is handled with the greatest possible care.