For decades, we have viewed weight loss as a grueling battle of wills. The common wisdom was simple: shedding pounds meant counting calories and outlasting your own biology through sheer grit. If the scale didn't move, it was seen as a personal failure or a lack of discipline to ignore the "food noise" buzzing in the brain. However, the rise of modern GLP-1 medications like semaglutide and tirzepatide has changed the conversation. These drugs reveal that hunger isn't just a mental state; it is a complex physical loop between the gut and the brain.
These medications don't use magic to "mute" your cravings. Instead, they step in and manage a physical process the body usually handles on its own. By mimicking a natural hormone, they change how your digestive system deals with a meal, turning the stomach into a slow-release tank rather than a high-speed hallway. To understand how they work, we have to look past the idea of "killing the appetite" and move toward the mechanics of how the body measures fullness through pressure, hormones, and timing.
The Plumbing of Fullness and the Gastric Speed Limit
In a normal digestive cycle, the stomach acts as a holding tank where food is broken down by acid and enzymes. It then moves into the small intestine through the pyloric sphincter, a muscular valve that acts as a gatekeeper. This gate opens and closes rhythmically to let small amounts of "chyme" (partially digested food) pass. Without medication, this process is fairly quick. Your stomach empties a few hours after a meal, eventually signaling the brain that it is ready for more.
GLP-1 medications change these rules by significantly slowing down "gastric emptying." When these drugs bind to receptors in the digestive tract, they tell the stomach to hold onto its contents for much longer. This isn't a minor tweak; it is a total change to the speed limit of your internal plumbing. Because food stays in the stomach for an extended time, its muscular walls remain stretched. This physical stretching is the main reason users feel full long after they have finished their last bite.
The Vagus Nerve: A Physical Message of Satiety
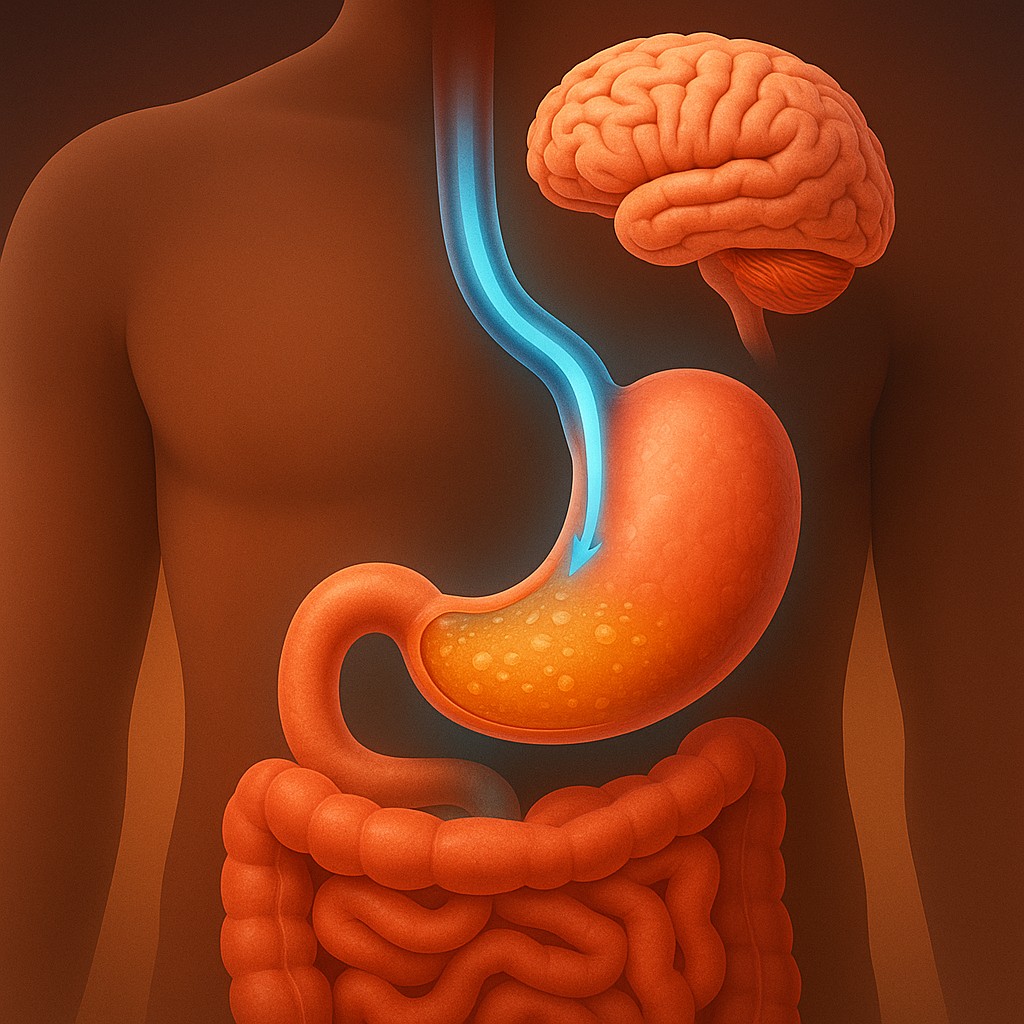
To understand why a slow stomach leads to a quiet brain, we have to look at the vagus nerve. This is the longest and most complex nerve in the body, acting like a high-speed fiber-optic cable that connects the gut directly to the brain’s command center. When food expands the stomach, specialized stretch receptors in the lining activate. They send a steady stream of electrical signals up the vagus nerve to the hypothalamus, the part of the brain that manages thirst, temperature, and hunger.
When the stomach empties quickly, those signals stop, and the brain starts looking for more energy. But because GLP-1 drugs keep the stomach full for hours or even days longer than usual, the vagus nerve keeps shouting "We're full!" to the brain. This creates "mechanical satiety," or fullness based on physical space. It is much harder to be tempted by a pastry or a second helping of pasta when your brain is getting a high-priority notification that there is simply no more room in the tank. This physical reality overrides mental cravings, effectively turning off the "food noise" that many people live with every day.
Comparing Natural and Medicated Digestion
The difference between how the body processes a meal naturally versus with GLP-1 is dramatic. Here is how the timing and physical sensations shift:
| Feature |
Natural Digestion |
GLP-1 Assisted Digestion |
| Stomach Emptying Rate |
Fast (usually 2 to 4 hours) |
Greatly Delayed (can be several hours longer) |
| Main Fullness Signal |
Brief hormone spikes |
Lasting physical stomach stretching |
| Vagus Nerve Activity |
Short bursts of "fullness" |
Constant stream of "fullness" |
| Return of Hunger |
Quick return as the stomach clears |
Very slow return; low appetite for long periods |
| Result of Overeating |
Bloating or mild discomfort |
Intense nausea and possible vomiting |
The Physical Cost of Ignoring the Gatekeeper
One of the biggest lessons patients learn on these medications is that the body no longer tolerates "eating through the fullness." Naturally, many people can ignore the first signs of being full and keep eating, perhaps finishing a large dessert even when the stomach is technically packed. This happens because the brain's reward system can sometimes shout louder than the stomach. However, when the stomach is slowed down by medication, these physical limits become rigid. If the stomach is full and hasn't moved its contents forward yet, adding more food creates a mechanical backup.
This backup is the main cause of the nausea people feel on these drugs. When the stomach cannot move food forward and a person keeps eating, the body has only one way to relieve the pressure: signaling nausea or triggering the gag reflex. This works as a powerful form of biological training. Over time, a person’s behavior changes because the "cost" of eating too much or too fast becomes physically painful. The stomach effectively dictates the pace of the meal, forcing a slower, more mindful approach.
Beyond the Stomach: Shifting Brain Priorities
While the physical slowing of the stomach is the most direct effect, it triggers a chain reaction in the brain’s reward system. Humans are wired to find high-calorie foods "rewarding." When we see something sugary or fatty, our brain releases dopamine, encouraging us to eat it so we can survive. However, when the vagus nerve is constantly telling the brain the stomach is full, the perceived value of that food drops. A slice of pizza that looked like a prize twenty minutes ago can suddenly look unappealing or even gross.
This shift explains why people on these drugs often see their tastes change. They may start choosing lighter, simpler foods because the heavy, rich meals they once loved now feel like "too much" for their slowed-down system. By changing the physical state of the stomach, the medicine recalibrates what the brain wants. It moves the needle from "I need to eat everything" to "I have enough energy, and I don't need to worry about the next meal."
A New View of Metabolic Health
Moving from viewing weight loss as a mental struggle to seeing it as a physical process offers a more compassionate, scientific perspective. By understanding that hunger is tied to how food moves through us, we can stop blaming ourselves for "weakness." Instead, we can appreciate the complex signals that keep us balanced. These medications are not a shortcut; they are a tool that resets the gut-brain connection. This gives people a chance to build new habits without the constant interference of an overactive hunger drive.
As we learn more about metabolic science, the lesson stays the same: our bodies are masterpieces of communication. When we listen to the physical signals of fullness and respect the pace of our internal systems, we gain a level of control that willpower alone cannot provide. Whether through medication, high-fiber diets that naturally slow the gut, or mindful eating, the goal remains the same: to find a rhythm where the body feels nourished, satisfied, and at peace.